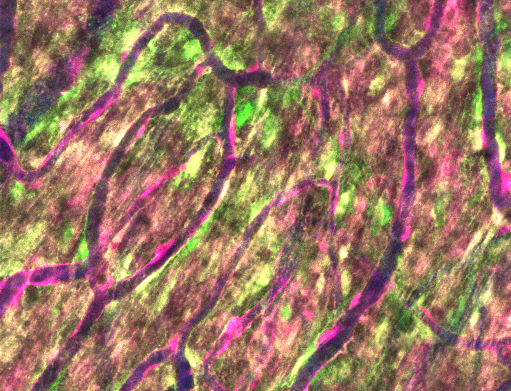
Congratulations to Stephanie Bonney for a new publication on perivascular fibroblasts. Direct link to PDF.
Perivascular fibroblasts (PVFs) are a specialized cell type enwrapping large parenchymal vessels in the central nervous system (CNS). Despite their prevalence in the neurovascular unit, the function of PVFs in normal physiology and pathophysiology remain poorly understood. Very recent studies have shed light on PVFs as contributors to scar formation and perivascular pathology in neurodegenerative diseases and brain injury1-4. However, there is still confusion in the field about how to distinguish PVFs from mural cells, as they occupy a common perivascular space, have similar appearance, and express some of the same molecular markers. In vivo two-photon imaging overcomes these issues and is poised to be an essential tool to study PVF biology. It provides the ability to define vascular cell characteristics at high-resolution in intact 3-D vascular architecture on the living brain over time. Our paper describes the transgenic mouse lines and distinct features of PVFs needed to elucidate their roles in vivo.
We demonstrate that PVFs coexist side-by-side with mural cells in the CNS. PVFs have a unique organization along the vascular tree in the healthy brain, wherein they localize specifically to penetrating arterioles, their pre-capillary offshoots, and larger ascending venules, but are absent from capillaries and smaller venules. We further show morphological distinctions between mural cells and PVFs with high-resolution in vivo imaging and complementary histology. Finally, we use longitudinal tracking to show that PVFs, unlike mural cells, display short-range mobility along the vessel wall in the healthy adult brain. Thus, PVFs and mural cells are distinct cell types coexisting in a common perivascular niche. These delineations provide the foundation to better understand the physiological and pathological roles of PVFs using in vivo imaging.
- Månberg A, Skene N, Sanders F, et al. Altered perivascular fibroblast activity precedes ALS disease onset. Nat Med. Apr 2021;27(4):640-646. doi:10.1038/s41591-021-01295-9
- Dorrier CE, Aran D, Haenelt EA, et al. CNS fibroblasts form a fibrotic scar in response to immune cell infiltration. Nat Neurosci. Feb 2021;24(2):234-244. doi:10.1038/s41593-020-00770-9
- Yahn SL, Li J, Goo I, Gao H, Brambilla R, Lee JK. Fibrotic scar after experimental autoimmune encephalomyelitis inhibits oligodendrocyte differentiation. Neurobiol Dis. 02 2020;134:104674. doi:10.1016/j.nbd.2019.104674
- Vanlandewijck M, He L, Mäe MA, et al. A molecular atlas of cell types and zonation in the brain vasculature. Nature. 02 2018;554(7693):475-480. doi:10.1038/nature25739